Decompression of lumbar spinal stenosis using the traditional laminectomy technique leads to good improvement of neurogenic claudication symptoms. However, impairment of facet joint and posterior tension band integrity can result in segmental instability and a significant reoperation rate, particularly when the spinal stenosis is associated with a spondylolisthesis, write Roger Härtl and Karsten Schöller. A minimally invasive unilateral laminotomy with “over the top” decompression is an attractive alternative because it limits trauma to the paravertebral muscles and facet joints and, on the same hand, permits sufficient and clinically effective bilateral neural decompression.

Lumbar spinal stenosis is a common condition in the elderly population, with growing socioeconomic importance. Typical symptoms like low back pain, leg pain and neurogenic claudication may have a dramatic impact on mobility and quality of life. Treatment options include surgical management aiming at decompression of the neural elements, as well as conservative management. A conservative trial is generally accepted in patients without severe neurological deficits; however, class I evidence data meanwhile clearly support the superiority of surgical over nonsurgical treatment.1 Similar findings have been reported for the combination of lumbar spinal stenosis with degenerative spondylolisthesis.2
The traditional laminectomy technique allows wide surgical decompression of the cauda equina, but has some known disadvantages: extensive tissue trauma and secondary instability contribute to a poor outcome in up to 50% of patients. Furthermore, the reoperation rates for fusion surgery are high, particularly in patients with additional spondylolisthesis. This is why—in this specific constellation—laminectomy plus additional fusion surgery has for a long time been regarded as the gold standard by many authors, against which all other techniques had to be compared. However, recent publications from Ghogawala et al3 as well as Försth et al4 in the New England Journal of Medicine (see front page, SN39, for a report and interview with Peter Försth12) could not demonstrate a significant overall benefit with the addition of spinal fusion to laminectomy, while indicating a reoperation rate of up to 34% after laminectomy alone. But what is the alternative to laminectomy for decompression of lumbar spinal stenosis with or without spondylolisthesis?
Minimally invasive spinal surgery has become increasingly common over the past two decades, as the usage of new surgical devices and techniques has evolved. In 1997, Spetzger et al first described unilateral laminotomy for bilateral or “over the top” decompression of the lumbar spine in a study detailing both surgical anatomy and clinical experiences,5,6 followed by McCulloch and Young a year later.7 These studies showed that bilateral decompression of the lumbar spinal canal is practical via a unilateral laminotomyusing microsurgical technique. The traditional subperiosteal midline access was subsequently modified by a transmuscular technique that utilises tubular retractors. The tubular access not only maximally protects muscle tissue and tendon attachments, it also offers particular advantages when treating obese and elderly patients. Furthermore, biomechanical testing has shown that minimally invasive tubular decompression causes less destabilisation compared with open laminectomy,8 and clinical data from our workgroup indicate an encouragingly low reoperation rate for spinal fusion.9 But is the minimally invasive unilateral technique as effective as the standard laminectomy and what is the advantage?

To answer these questions, our workgroup performed a systematic review and a meta-analysis to compare reoperation rates and patient satisfaction after minimally invasive unilateral laminotomy with “over the top” decompression and open laminectomy that was recently accepted for publication in Neurosurgery.10 Thirty-seven studies and 1,156 patients with lumbar spinal stenosis plus spondylolisthesis were included in our analysis. After minimally invasive decompression we found an overall reoperation rate of 5.8% and a reoperation rate for spinal fusion of 3.3%, which was considerably lower than after laminectomy (16.3% and 12.8%, respectively). Furthermore, we found a higher patient satisfaction after minimally invasive decompression (76%) compared to open laminectomy (62.7%). These data show a clear advantage of the minimally invasive technique over the traditional technique. But how can one adopt this technique to his practice?
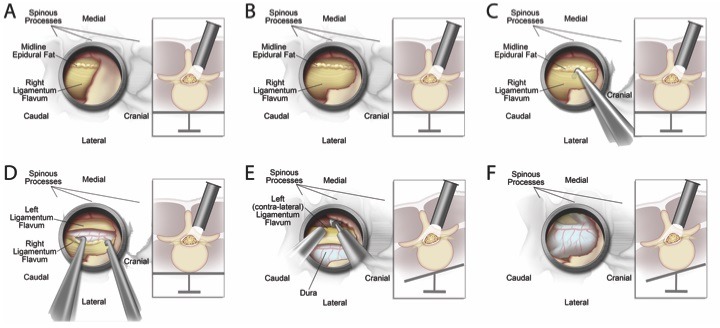
Our manuscript, titled “Ten-Step MIS Lumbar Decompression and Dural Repair through Tubular Retractors”,11 which has also been accepted for publication in Neurosurgery, reviews our experience from 2008 to 2014 developing a step-by-step description of the surgical techniques (Figure 1 details the steps of the minimally invasive decompression technique from unilateral laminotomy to “over the top” decompression) and complication management, including Dural repair through tubes, for the four lumbar pathologies of highest frequency including minimally invasive unilateral laminotomy. Our overview and complementary material document the key technical details to maximise the success of these four minimally invasive surgical techniques. The review of our experience in 331 patients reveals technical feasibility as well as satisfying clinical results, with zero postoperative complications associated with cerebrospinal fluid leaks, one infection, and 17 instances (5.1%) of delayed fusion.
In conclusion, according to our data minimally invasive unilateral laminotomy is a good alternative to laminectomy with advantages regarding reoperation rate and patient satisfaction. It may also even be a more cost-effective alternative to fusion surgery, with a lower complication rate. Minimally invasive surgery through tubular retractors is a safe and effective alternative to traditional open techniques for the treatment of lumbar degenerative disease. Adherence to strict microsurgical techniques will allow the surgeon to effectively address bilateral pathology while preserving stability and minimising complications.
Roger Härtl is a professor of neurological surgery, the director of spinal surgery and the co-director of the Weill Cornell Spine Center, New York City, USA. Karsten Schöller is the head of spinal surgery at Justus-Liebig-University Giessen, Giessen, Germany.
References
- Weinstein, J. N. et al. Surgical versus nonsurgical therapy for lumbar spinal stenosis. N. Engl. J. Med. 358, 794–810 (2008).
- Weinstein, J. N. et al. Surgical versus nonsurgical treatment for lumbar degenerative spondylolisthesis. N. Engl. J. Med. 356, 2257–2270 (2007).
- Ghogawala, Z., Dziura, J., Butler, W. & Et Al. Laminectomy plus Fusion versus Laminectomy Alone for Lumbar Spondylolisthesis. N. Engl. J. Med. 374, 1424–34 (2016).
- Försth, P., Ólafsson, G., Carlsson, T. & Et Al. A Randomized, Controlled Trial of Fusion Surgery for Lumbar Spinal Stenosis. N. Engl. J. Med. 374, 1413–23 (2016).
- Spetzger, U., Bertalanffy, H., Reinges, M. H. & Gilsbach, J. M. Unilateral laminotomy for bilateral decompression of lumbar spinal stenosis. Part II: Clinical experiences. Acta Neurochir. (Wien). 139, 397–403 (1997).
- Spetzger, U., Bertalanffy, H., Naujokat, C., von Keyserlingk, D. G. & Gilsbach, J. M. Unilateral laminotomy for bilateral decompression of lumbar spinal stenosis. Part I: Anatomical and surgical considerations. Acta Neurochir. (Wien). 139, 392–6 (1997).
- McCulloch, J. A. Essentials of spinal microsurgery. (Lippincott Raven, 1998).
- Bresnahan, L., Ogden, A. T., Natarajan, R. N. & Fessler, R. G. A biomechanical evaluation of graded posterior element removal for treatment of lumbar stenosis: comparison of a minimally invasive approach with two standard laminectomy techniques. Spine (Phila. Pa. 1976). 34, 17–23 (2009).
- Alimi, M., Hofstetter, C. P., Pyo, S. Y. & Paulo, D. Minimally invasive laminectomy for lumbar spinal stenosis in patients with and without preoperative spondylolisthesis: clinical outcome and reoperation rates. J NeurosurgSpine. 2015 Apr;22(4):339-52.
- Schöller, K., Alimi, M., Cong, G.-T., Christos, P. J. & Härtl, R. Lumbar Spinal Stenosis Associated With Degenerative Lumbar Spondylolisthesis: A Systematic Review and Meta-analysis of Secondary Fusion Rates Following Open vs Minimally Invasive Decompression. Neurosurgery accepted for publication, (2016).
- Boukebir, M. A. et al. Ten-Step MIS Lumbar Decompression and Dural Repair through Tubular Retractors. Neurosurgery accepted for publication, (2016).
- Hignett, KR. Adding fusion to decompression fails to improve clinical outcomes in treatment of lumbar stenosis. Spinal News International. 38, (2016).
Roger Härtl is a professor of neurological surgery, the director of spinal surgery and the co-director of the Weill Cornell Spine Center, New York City, USA. Karsten Schöller is the head of spinal surgery at Justus-Liebig-University Giessen, Giessen, Germany.













