 Sacroiliac joint fusion surgery has grown in popularity over the past five years. Whilst procedure rates are still relatively low, many physicians are convinced of the surgery’s benefit for the treatment of pain generated in the sacroiliac joint. With treatment guidelines from the North American Spine Society and the International Society for the Advancement of Spinal Surgery, as well as new payment recommendations from US Medicare, sacroiliac joint fusions surgery is set to become more common than ever before. Donald Hales, Steven Garfin, Louis Rappoport, Michael Barnum and Choll Kim speak to Spinal News International about sacroiliac joint fusion surgery, and compare some of the different devices available for the procedure.
Sacroiliac joint fusion surgery has grown in popularity over the past five years. Whilst procedure rates are still relatively low, many physicians are convinced of the surgery’s benefit for the treatment of pain generated in the sacroiliac joint. With treatment guidelines from the North American Spine Society and the International Society for the Advancement of Spinal Surgery, as well as new payment recommendations from US Medicare, sacroiliac joint fusions surgery is set to become more common than ever before. Donald Hales, Steven Garfin, Louis Rappoport, Michael Barnum and Choll Kim speak to Spinal News International about sacroiliac joint fusion surgery, and compare some of the different devices available for the procedure.
What is the current state of sacroiliac joint fusion surgery?
Donald Hales: It has been estimated that up to 18% of low back pain may be related to dysfunction of the sacroiliac joint (SIJ). Although chiropractic and osteopathic physicians have long recognised this in their practices, orthopaedic surgeons are onl
y just becoming aware of this phenomenon.
There has been a growing awareness over the past five years of the pain that the SIJ can generate and of new minimally invasive surgical treatments when non-operative care has failed. As training has occurred and a few papers have been presented at meetings, awareness has increased. More surgeons are becoming convinced that the SIJ can be a significant pain generator, and treated operatively if necessary.
Steven Garfin: The sacroiliac joint was not something I paid attention to until around 2009. Similar to non-specific low back pain, there are not a lot of definitive tests that say, “Yes, the sacroiliac joint is causing this patient’s back pain”.
We are struggling with a lack of awareness of the possibility that pain is coming from the SI joint. Adoption is slower than I had expected, but awareness—and appropriate treatments—are expanding.
Louis Rappoport: Physicians do not feel comfortable making the diagnosis, I think, because we very rarely see anything significant on imaging tests. I think that the key is to listen to the patient. Groin pain, for example, is a very common presentation which only usually comes from an SIJ problem or degenerative arthritis of the hip.
Donald Hales: Along with the history and positive physical exam findings, painful SIJs are usually injected with a long-acting local anaesthetic. If the patient experiences a significant reduction in symptoms following the injections it is considered as being confirmatory of the SIJ as being a main pain generator for the patient. Of course, it may not be the only pain generator.
Aside from physician awareness and diagnosis, what are the biggest challenges facing SIJ fusion surgery?
Michael Barnum: A big educational challenge is the radiographic visualisation of the sacrum and sacroiliac joint during the procedure. I would highly recommend going to a cadaver course to get “hands-on” experience prior to performing the procedure, and having someone proctor your first cases.
Choll Kim: The radiographic imaging not only varies from patient to patient, but it is relatively unfamiliar to most spine surgeons.
Steven Garfin: Another big challenge has been getting American Medical Association coding for minimally invasive SIJ procedures. Now that it has a Category I code, it is becoming more accepted. Both NASS and ISASS have published positive coverage recommendation policies. These changes, coupled with more and more published data, have resulted in Medicare establishing positive coverage policies in most US states (see page 19), which was a big hurdle. The next hurdle will be establishing payment among the commercial insurance companies and that should occur as longer term data gets published.
Louis Rappoport: I have a lot of unhappy patients that want the procedure but cannot have it done because their insurance does not cover it. Medicare, however, is coming around to the idea, and is paying for the procedures in most regions. As we get more outcomes data, insurance companies will be more likely to start approving the procedure.
Donald Hales: Despite being cleared by the US Food and Drug Administration (FDA) as safe and effective in treating SIJ pain, some insurance providers label it as “experimental”, clearly using their own definitions. Surgeons may need to do peer-to-peer reviews with medical directors, or even go through a three-level appeals process to ultimately get authorisation to perform the procedure.
Steven Garfin: The biggest challenge, however, remains the acceptance of the concept that the SI joint can be a cause of pain. It has been so long ingrained that the SI joint is not a pain generator that some surgeons still dismiss it.
The iFuse platform is by far the most commonly used sacroiliac joint fusion system on the market. Steven Garfin discusses the product’s benefits, and the research base behind it.
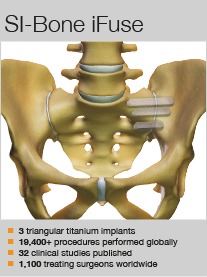 What is your experience of the iFuse?
What is your experience of the iFuse?
Steven Garfin: I was one of the first people outside of its inventor to use it, and I got involved with some of the national clinical trials. Because of this, I could not personally perform another procedure, as per my institution’s rules for national principal investigators. However, I have three partners who do these cases; I know what they are doing, I know the results. I go to many spinal meetings throughout the year and present on the diagnosis and clinical results. However, what I discuss is not from my own experience of performing the procedure.
So, what does the data show?
Steven Garfin: In general, the results have been very good. But, one has to use data appropriately. It works well—when the clinical diagnosis and tests are done correctly—but that may not always be the case. When all of the pre-operative criteria are right, however, and the implants are placed correctly, the improvements in pain and function are really very good.
What are its key benefits?
Steven Garfin: First, it has been available for a while and surgeons know how to use it. The iFuse has the longest track record. The technique is like treating a fractured hip; the steps are similar, and orthopaedists have experience in other areas of the body with tools like this.
Two, it is has very good data. Most of the current SI fusion data relates to the iFuse device; we know what to expect. Other devices may be okay, too, but they just don’t have the traction, the experience and the clinical database behind them.
Lastly, the implants are very stout; they hold up, and they do not break.
Steven Garfin is a professor and chairman of the Department of Orthopaedics at the University of California; he is the chair of the SI-Bone Surgeon Advisory Board
Offering a different approach to sacroiliac joint fusion surgery, the Zyga SImmetry device uses a decortication process in order to better promote intra-articular fusion.
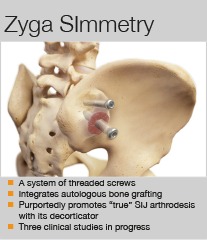 What are its key benefits?
What are its key benefits?
Donald Hales: This system allows for rigid fixation with two large threaded screws across the SIJ, as well as a system of flexible bone rasps that are introduced into the joint to decorticate the joint surface. This removes the cartilage surface of the joint. Bone graft is then introduced into the joint to stimulate the bony surfaces to heal together, causing a fusion. Without a fusion there is the risk of the implanted hardware loosening up over time, and the possibility of losing the initial benefit of the surgery.
What complications could occur during this procedure?
Donald Hales: As a minimally invasive procedure the complications are few. A potentially serious complication would be a mal-positioned screw, which could lead to the injury of a major blood vessel inside the pelvis, and a catastrophic loss of blood with the need for transfusions or vascular surgery to repair the injury.
A more likely complication is nerve injury from a screw placed into the S1 or S2 foramen. Accuracy of screw placement is dependent on good imaging during surgery, for example with intraoperative fluoroscopy via a C-arm. C-arm imaging can, however, be degraded with obesity, or by human error. I have been working on a surgical technique to rapidly and accurately place screws using 3D navigation systems, which should allow surgeons to confidently place guidewires, which can then guide the screws home safely. I think this technique will be adopted by surgeons once they have been exposed to educational opportunities.
Donald Hales is an orthopaedic surgeon at Northern Arizona Orthopaedics, Flagstaff, USA, and a consultant for Zyga
Made of dense cancellous bone, the SI Fix implants from NuTech can be used as an alternative to metal implants. Given their allograft composition, they should not need to be removed, potentially eliminating the revision surgeries associated with metal implants.
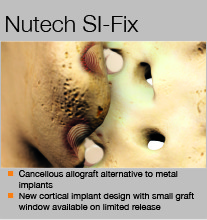
What are its key benefits?
Choll Kim: The key benefit of the SI Fix is that is represents a minimally invasive strategy of a traditional fusion strategy. It is equivalent to an interbody fusion, which remains the best method of arthrodesis. In addition, the use of a structural allograft offsets the issues related to implant failure. The ability to work in line with the joint provides a distinct advantage of SI Fix over the percutaneous transarticular fixation systems currently available for minimally invasive treatment.
Have you experienced any problems with this device?
Choll Kim: The challenge with all SI fusion strategies, whether intraarticular or transarticular, is related to the variability of the SI joint itself. I am surprised how different the morphology of the SI joint can be from patient to patient. The unique anatomic characteristics of the SI joint mandates that care be taken when placing implants to stabilise the motion segment.
Choll Kim is an orthopaedic spinal surgeon at the Spine Institute of San Diego, San Diego, USA. He is a paid consultant for NuTech
 What is your experience of the Globus SI-Lok?
What is your experience of the Globus SI-Lok?
Louis Rappoport: After using the iFuse for a while, I became unsatisfied with the fact we were impacting something quite vigorously across the joint, and expecting bone to grow back to the device. In my own practice I saw a significant loosening issue on the sacral side. After a while, I decided to switch over to the SI-Lok. With a screw device you are not destroying bone material by impaction. You’re threading something across the joint, which made more sense to me.
Michael Barnum: I was on the design team for the system, which I have been using since its FDA approval. Prior to using SI Lok, I used the iFuse device. I have taught courses for both. I have performed over 200 SIJ fusion surgeries.
What are its key benefits?
Michael Barnum: The SI Lok system screws have hydroxyapatite coating and slots that cross the SI joint. Regarding fusion, you usually get initial fixation with the screws there. You get bone growth through the slots, then bony ingrowth into the screws themselves, and finally auto fusion of the joint.
Louis Rappoport: The slot allows bone to grow across the device at the level of the joint. No matter what device we use, we never see true fusion of the joint. Really, we are stabilising the joint, and trying to get implants permanently fixed across it.We get limited fusion across the slot, and that is the goal.
Have you experienced any problems with this device?
Michael Barnum: If someone develops a non-union of the sacroiliac joint, then the screws can be difficult to get out with the bony ingrowth into the hydroxyapatite coating.
Louis Rappoport: The mechanical forces across the sacroiliac joint are tremendous; it basically transfers force from the torso onto the pelvis and across the lower extremities. The sacral bone in the majority of patients tends to be somewhat spongey, whilst the iliac bone is much better. Because of these factors, we typically see screws and implants becoming loose on the sacral side. I think that we are still in early evolution of these devices. We still have a long way to go.
Michael Barnum is an orthopaedic surgeon at Northwestern Medical Center, Saint Albans, USA. Louis Rappoport is an orthopaedic surgeon at Arizona Spine Consultants, Phoenix, USA. Both hold paid consulting positions with Globus Medical













