A team lead by Denis Evseenko (Department of Orthopaedic Surgery, University of Southern California, Los Angeles, USA) hopes to delay or reduce the need for joint replacement surgery in osteoarthritis patients with an injection.
Osteoarthritis is also known as degenerative joint disease. It is a condition in which the protective cartilage that cushions the tops of bones degenerates, or wears down, causing swelling and pain. It may also cause the development of osteophytes, or bone spurs. When osteophytes develop in the spine, the spurs can put pressure on the nerves leading to the spinal column. This can cause weakness and pain in the arms or legs.
When osteoarthritis worsens, joint replacement surgery is often the only option for patients. Although these procedures are well established, some people—especially younger patients—end up with limited mobility, or they eventually progress to the point where additional surgeries are needed.
In a new publication in the Annals of Rheumatic Diseases, Evseenko and colleagues describe the promise of a new molecule called Regulator of Cartilage Growth and Differentiation, (RCGD 423). The drug works on the body’s glycoprotein 130 receptor, which receives two types of signals that either promote cartilage development or trigger chronic inflammation. RCGD 423 enhances the reception of the cartilage growth signals while blocking the inflammatory ones that lead to degeneration.
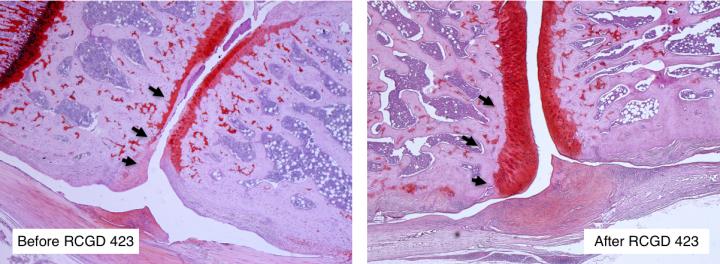
The researchers found that during in vitro studies, the drug helped joint cartilage cells proliferate. When they injected RCGD 423 into mice, they observed improved healing of cartilage damage.
Evseenko comments: “The goal is to make an injectable therapy for an early to moderate level of arthritis. It’s not going to cure arthritis, but it will delay the progression of arthritis to the damaging stages when patients need joint replacements, which account for a million surgeries a year in the USA”
Because there is no cure for osteoarthritis, the only options for patients are cartilage replacements and treatments that help manage symptoms. Several companies are working on next-generation treatments, including Hyalex Orthopaedics, which is developing a synthetic biomaterial that mimics cartilage. Centrexion Therapeutics is working on novel pain-relieving therapies, and Servier recently licensed a therapy from Galapagos that targets a cartilage-degrading enzyme called ADAMTS-5.
Evseenko is also looking at other alternatives to joint-replacement surgery, including using pluripotent stem cells to regenerate cartilage.
As Evseenko sees it, the potential of RCGD 423 does not only lie in arthritis—it could lead to an entirely new class of anti-inflammatory drugs. In a previous study published in Nature Cell Biology, RCGD 423 was shown to activate hair growth. His team has developed several similar drugs and is partnering with other scientists to explore their applications in rheumatoid arthritis, lupus, neurological and heart diseases.













