
Three-dimensional printing—also known as additive manufacturing—is one of the most exciting platforms shaping technology across sectors as diverse as art, food production and medicine. In play since the early 1980s, it is only in recent years that the potential of 3D printing has begun to receive mainstream attention. From the development of artificial skin for burn victims to the development of bionic ears, additive manufacturing offers an unimaginable array of possible applications in medicine. In this feature, we take an in-depth look at the ways in which additive manufacturing is transforming spinal surgery from the perspectives of physicians.
Ralph Mobbs, a neurosurgeon from Sydney, Australia, has pioneered the use of 3D printing in the creation of patient-specific spinal implants. He takes us through the current state of the art, future applications in the spinal field and beyond, as well as one of his most exciting cases so far.
How does the process of creating a personalised implant with a manufacturer work? How much input does the physician have?
Creating a personalised patient specific implant can take quite some time, however the process will speed up significantly as we get more experienced with the workflow involved.
The first step is for the surgeon to identify the patient who may benefit from such an implant. We require high-quality imaging of the patient, usually a fine cut computed tomography (CT) scan, so that an accurate 3D computer-aided design model can be created. We will be able to do this modelling using magnetic resonance imaging scans with bone algorithms in the future; however, this is still in development.
The second step is for the surgeon to connect with a computer-aided design engineer. It is up to the surgeon to interpret the 3D computer-aided design imaging models to assist the engineer to identify what structures will need to be removed, and subsequently reconstructed.
Thirdly, the engineer and surgeon combine to design and slowly build an implant using the computer-aided design software that will go into the defect that needs to be reconstructed. The surgeon needs to be mindful of how the implant will be implanted, the regional anatomy, and of course ‘bail-out’ options should the procedure not go to plan.
I predict that, in the future, we will have modelling software on a surgeons’ desktop so that they can perform the function of the engineer, with minimal delays, so that the design process can be sped up significantly.
After creating a patient-specific implant model on the computer-aided design software, it then gets a little more complicated!
We need to determine how much load will be transferred through the implant, and the various forces that the implant will need to accommodate and transfer. The model needs to have various details added. This includes the porous and endplate architecture, the lattice structure throughout the implant to transfer load, any other specific features that may assist with implantation and structural integrity of the construct, and the list goes on.
The surgeon and engineer need to work closely together, with both teams intimately involved with all phases of the implant design and construction.
Finally, the implant design goes to your local 3D printer to be made! There is some minor post-production detail and quality control, but it is now ready to be sterilised and implanted. Wasn’t that easy!
If you want a nice quick easy implant for your next case, get something “off-the-shelf”, as this process does take time and attention to detail.

How long has it taken, in your experience, from patient consultation to the actual implantation?
I have been involved in a number of cases to date, with the first implant taking about two months to plan, print, and finally get to the operating room. We have sped up our processes significantly, and this is now reduced to a few weeks.
In the future, my prediction is that the time from patient consultation to implantation will go from weeks to days, and eventually to just hours. There will be a 3D printer in the corner of your operating room. If it does not perfectly fit, you will be able to print another one!
Imagine having a complex fracture with an anaesthetised patient on the operating table, and while you are doing the exposure, the prosthesis is being printed. We will get there—it is only a matter of time.
For a surgeon, what are the most satisfying parts of using a patient-specific 3D printed device in the operating room?
I cannot relate in words how satisfying it is to do a complicated operation that is stressful and time-consuming, when, at the end of the procedure, you get to place a perfectly-fitted, patient-specific implant. It is just a beautiful thing.
Do you think that there might be regulatory barriers to customised 3D implants?
Absolutely, yes. There is no current standardised framework for regulation of these implants. You may eventually get to a point where implants for various parts of the body need to reach certain mechanical loading parameters based on computer-aided design modelling. This has been a barrier to implementation, however, in my opinion, the benefits outweigh the risks of this technology at this point in time.
What are the most exciting benefits offered by 3D printing for spinal surgeons?
The capacity to design an implant that fits perfectly for a given situation is gold. You can dial up, or dial down, the degree of endplate porosity, depending upon what you want to achieve and the speed of osteointegration. The future will keep getting better!
In which circumstances is this technology most helpful?
Complex reconstructive operations are the target. The type of operation where there is not a convenient “off-the-shelf” pre-made implant option is the sweet spot. Cancers, trauma, and advanced degenerative conditions lend themselves nicely to this technology.
In the future, however, I am certain that any degenerative condition will benefit, whether it is hip and knee, or spine.
Case report
Mobbs performed a complete T9 vertebrectomy and T9-10 rib resection on a young, female patient with a tumour and pathological fracture, as well as sagittal and coronal deformity. The vertebrae was replaced with a patient-specific 3D-printed implant designed by Mobbs and his team, along with a manufacturing company. A number of porous titanium cages were designed prior to surgery with different size specifications. The final implant was 12mm with a large footprint. The surgery was completed successfully, with relatively minimal blood loss, no complications, and normal spinal cord functioning by the end of the case. Mobbs describes the specifics of the case and the pleasures of performing this kind of surgery with a perfectly-designed implant.
Last year, I had a girl in her mid-teens present with a very rare spinal tumour. She was not doing well. She had terrible mechanical pain in the back as one of her vertebrae was destroyed by the tumour, and progressive compression of the spinal cord. She had completed radiotherapy and chemotherapy, and her condition was deteriorating.
The difficulty, however, was that she not only had a destroyed vertebra, but her spine was bent forward and twisted to the side. She required a very major procedure—a wide tumour resection—but also a plan to put her back together again. A real challenge and something I love doing.
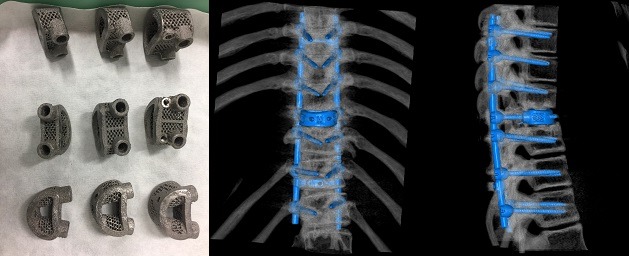
We worked out her operation using 3D computer-aided design software to plan the approach, plan the tumour resection and also plan the reconstruction. It sure is exciting to be able to do the operation on a computer before you go anywhere near the operating room! After planning the tumour resection and decompression of the spinal cord, we worked out the size and shape of the defect that we needed to reconstruct, and then got to work on designing the 3D patient-specific implant.
I worked with an engineer from ProCRO, a design firm that specialises in medical 3D printing. We printed several plastic models in various states of the surgical procedure, then designed the custom implant to mimic the normal height and angulation of the vertebrae on what we predicted it should look like before it was destroyed by the tumour. It was great to print an implant based on what the spine should look like, then go into the operating theatre and perform the procedure.
The surgery was beautiful. The implant slotted in like a key into a perfectly-fitted lock—just magical stuff. It really provides a huge leap forward in complex reconstructive surgery. This is the way of the future, no doubt about it. The patient recovered amazingly well, and was back on the netball court three months after surgery. There are so many benefits to using customised 3D implants, I would not know where to start…The custom prosthesis added significant value, not only with reduction in operative time, but with providing initial firm stability of the cancer segment and perfect.
What improvements need to be made within the market for these kinds of implants to become more widely used?
The first major issue is the time between the surgeon identifying the appropriate patient, and production of the final implant. It is lengthy; however, this time is being shortened rapidly.
Secondly, spinal implants are currently being printed out of titanium. We need to explore a whole new range of suitable biomaterials.
Finally, the expense profile of these implants makes them difficult to make a business case for, except where implants are being 3D printed for “off-the-shelf” use. Patient-specific implants will remain high cost until the speed of design and printing is significantly reduced.
What do you think are the next steps for this technology over the coming years?
The first step is to sure-up the regulatory framework. This needs to be sorted out rapidly for the ongoing uptake of patient-specific implants.
The next step is to expand the indications for using this technology. The primary use is for complex reconstruction, however, we will see more 3D-printed implants for routine procedures, whether for fusion or for motion-sparing disc replacement surgery.
Additive manufacturing is not just for patient specific implants, but can be also used for off-the-shelf applications. An example of this is the Stryker Tritanium range. They produce a 3D implant designed for excellent porosity, ease of implantation, and with a good radiological signature. The range is manufactured using 3D printing, however this is for high-volume use rather than for a single unique procedure.
Where else in medicine do you think 3D printing will have a big impact?
Everywhere and anywhere! At this point in time we are printing reconstructive implants however, in the future, we will likely print biological implants based on the patient’s own cell lines.
I predict that we will be using different forms of biomaterials for printing, and finally printing patients’ own cells onto a scaffold for new organs; printed skin, liver or a heart.
The future with 3D will just get more and more exciting.
Ralph Mobbs is a neurosurgeon at Prince of Wales Hospital, Sydney, Australia.













