A study led by the University of Hong Kong (HKU), Hong Kong, is first to report that a new biomarker—the ultra-short time-to-echo disc sign (UDS), imaged using ultra-short time-to-echo magnetic resonance imaging (UTE MRI)—is significantly related to degenerative spine changes, low back pain and disability, in comparison to conventional MR images. The research, which is the first to report this finding, was published in Spine.
Over the past decade, various novel MRI technologies have been developed in an effort to address more sensitive measures to assess spine degeneration. UTE MRI assesses MRI signal from short T2 components that are not detected on conventional T2-weighted MRI. It can be performed on any MRI machine and takes approximately 15–20 minutes to scan the lumbar spine of one individual, according to the authors. Utilising UTE MRI, the team has identified the UDS and evaluated its clinical importance.
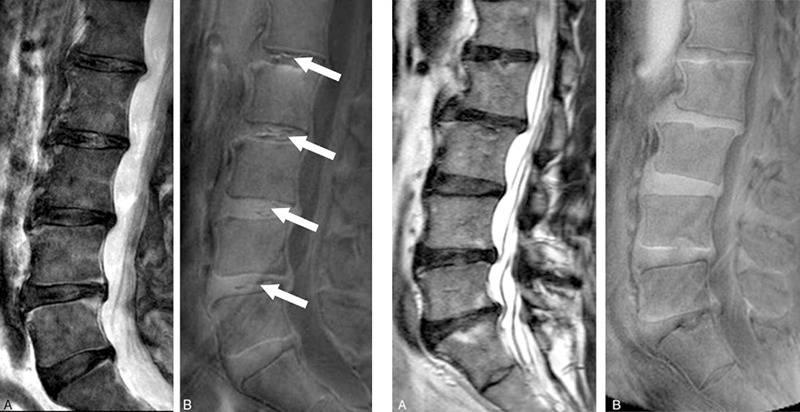
One hundred and eight southern Chinese participants were recruited (mean age: 52 years, equal number of male and female subjects). T2-weighted MRI was used to assess disc degeneration and other phenotypes, and T1-rho MRI values represented quantitative proteoglycan content of the disc. UDS was detected on UTE as a hyper- or hypo-intense band across a disc. The cumulative number of UDS levels represented a UDS score, whereas summated degenerated scores of lumbar levels via T2-weighted MRI represented a cumulative disc degeneration score. Subject demographics, low back pain every day (chronic) in the past year and disability profiles (Oswestry Disability Index, ODI) were obtained.
The UDS biomarker was found to be significantly related to degenerative spine changes, low back pain and disability in comparison to conventional MRI imaging.
The UDS was noted in 39.8% subjects, of which 61.4% occurred at the lower lumbar levels. Subjects with UDS biomarkers had significantly more disc degeneration and levels with pathologic changes of the vertebral bodies (ie. Modic changes). Based on disc levels, a higher prevalence of disc degeneration and disc bulges/protrusions, Modic changes and spondylolisthesis (ie. slippage of the vertebral body) were noted in UDS discs than non-UDS discs (p<0.05). T1-rho values were lower in UDS discs than non-UDS discs (p=0.022). The majority of UDS could not be detected on conventional T2-weighted MRI. The UDS score was significantly correlated with worse ODI scores (r=0.311; p=0.001) and pain (p=0.009), whereas T2-weighted cumulative disc degeneration score was not (ODI: r=0.13; p=0.19, low back pain: p=0.127). Thirty-nine point five per cent of UDS subjects who had multi-level involvement also had a higher prevalence of low back pain (p<0.015), however this correlation was not found on T2-weighted MRI (p=0.53).
According to lead investigator, Dino Samartzis, “Our study provides the ‘missing link’ between imaging findings of the spine and the development of low back pain and disability … Using UTE MRI has allowed us an opportunity to identify ‘hidden’ degenerative disc findings in an easy, quick and reliable fashion that helps us understand what is going on within the spinal discs much better than ever before. This has also led us to understand why someone may develop low back pain and if the pain may indeed have its ‘origins’ within the disc.”
First author, Henry Pang, further notes,“Among various MRI sequences, UTE MRI is the only sequence so far in our study that showed definite correlation between back pain, disability and degenerative disc changes. At the same time, as our study group unveils the previously hidden pathologies in traditional MRI, these findings may promote further understanding in the pathologies and therapies for low back pain and lumbar degeneration.”
Future study plans are underway to further investigate the relationship between the UDS biomarker and back pain.
Samartzis concludes, “This new imaging technology and the assessment of the UDS may supplement conventional MRI, therefore providing a larger snapshot into a patient’s spine degeneration and pain profiles … allowing clinicians to develop more personalised and precise management options to improve patient outcomes. This certainly represents a new leap forward in the visualisation of the spinal discs and perhaps pain.”













